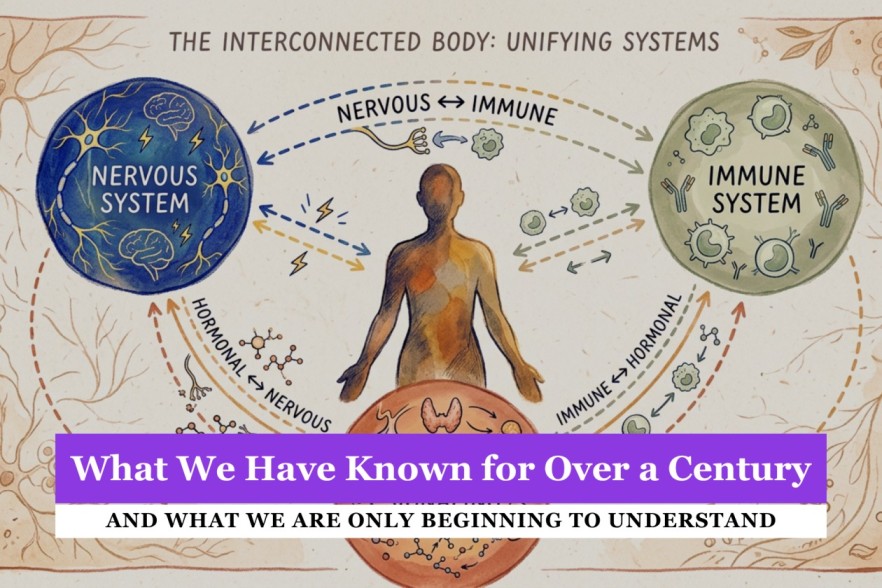
Biophysics Part 1
If biology operates according to physical laws, and it does, then understanding life requires more than chemistry alone. It requires understanding energy flow, signaling, and dynamic organization.
What was once dismissed as vague or unmeasurable is increasingly being explored through the lens of physics, systems biology, and biophysics.
This series begins with what science has known for over a century — and what we are only beginning to apply.
What Do We Mean by Energy?
When we talk about energy, most of us think in simple, everyday terms.

Do I feel energized when I wake up?
Do I move through my day with ease — or feel like I’m pushing through it?
Do I take the stairs, or look for the elevator — even going down a couple of flights?
This is the most familiar way we experience energy, how we feel, how we move, how we engage with life.
But this is only the surface.
The Energy You Don’t Feel
There is another layer of energy that operates entirely outside of our awareness.
At any given moment, your body is performing countless tasks:
- digesting food
- regulating blood sugar
- coordinating immune responses
- repairing tissues
- maintaining temperature
- transmitting signals between cells
You are not consciously directing any of this.
And yet, it requires energy, continuously.
The question is not simply:
“Do I feel energized?”
But also:
“Does my body have the capacity to perform the countless functions required to maintain balance and adapt to change?”
Because these two are connected, but they are not the same.
You can feel “fine” while deeper systems are under strain.
And you can feel fatigued when those systems are struggling to keep up.
A Different Way to Think About Energy
When we begin to look more closely, energy in the body is not just about how much we have.
It is about how it is:
produced
distributed
and used
It is about coordination.
It is about whether the systems of the body are working together effectively — or not.
From Experience to Science
This brings us to a deeper question:
What is energy, really?

In everyday language, we think of it as something we “have” or “don’t have.”
But in science, energy is understood differently.
It is not a feeling.
It is not a metaphor.
It is a fundamental property of the physical world, the capacity for movement, change, and interaction.
At the beginning of the 20th century, scientists began to study this in ways that would fundamentally change our understanding of matter itself. Researchers like Max Planck, Albert Einstein, Niels Bohr, and Erwin Schrödinger demonstrated something that was both precise and unsettling:
At its most fundamental level, matter is not solid in the way we perceive it.
It is dynamic. It is energetic. It is governed by patterns of interaction.
This is not new science.
It is over one hundred years old.
For many outside the field of physics, these ideas became accessible through works like The Dancing Wu Li Masters by Gary Zukav, which helped translate complex discoveries into language that non-scientists could begin to grasp.
What emerged was not mystical, but it was unfamiliar:
The world at its most fundamental level does not behave like a machine.
It behaves like a dynamic interplay of energy, probability, and interaction.
From Physics to Biology
It is easy to think of physics and biology as separate domains.
But they are not.
Biology does not operate outside the laws of physics.
It is an expression of them.
Every cell in the human body exists within this same reality:
electrons move
gradients form
signals are transmitted
energy is transformed
What we call “biology” is, in many ways, the organized expression of these processes.
Over time, entire fields have emerged to study this integration, including Biophysics and Systems Biology, disciplines that examine how living systems function as coordinated, interacting networks rather than isolated parts.
This perspective does not replace what we already know.
It expands it.
Understanding the Body as a System
For much of modern medical history, the human body has been studied through a reductionist lens, breaking complex systems into smaller and smaller parts in order to understand them.
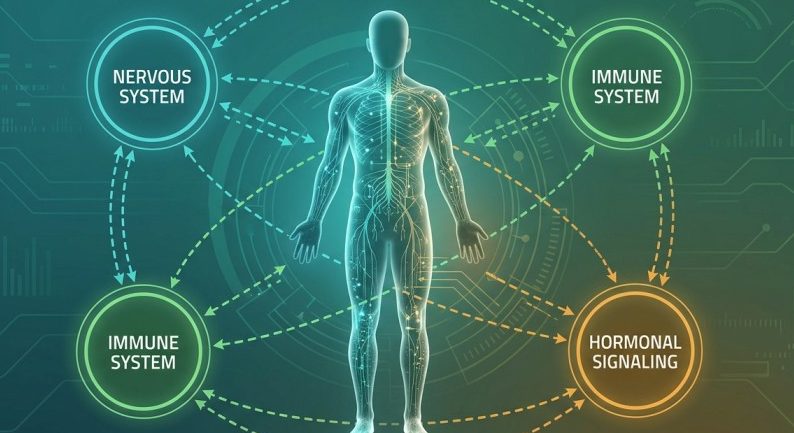
This approach has been extraordinarily useful.
But it has limits.
Because living systems do not behave like machines assembled from independent components.
They behave like dynamic networks, constantly communicating, adapting, and responding.
One of the clearest demonstrations of this came from the field of Psychoneuroimmunology, pioneered by researchers such as Robert Ader and Nicholas Cohen.
Their work showed that the systems of the body are not separate — they are in constant communication.
For example:
The brain influences the immune system
Think about what happens during prolonged stress.
Deadlines pile up. Sleep becomes disrupted. The mind is constantly engaged.
After a period of sustained stress, many people notice something familiar:
They get sick.
A cold appears. An infection lingers.
This is not coincidence.
Chronic stress signaling from the brain alters immune function, making the body less effective at responding to pathogens.
The immune system communicates back to the brain

Now consider the opposite direction.
When you have the flu, your experience is not limited to physical symptoms.
You feel:
fatigued
mentally foggy
withdrawn
uninterested in normal activity
That “sick feeling” is not just discomfort — it is communication.
The immune system releases signaling molecules that affect the brain, altering mood, energy, and behavior to support recovery.
Emotional stress alters immune function
Think of a time when you were going through a difficult emotional period:
conflict in a relationship
grief
ongoing worry
During these times, people often notice:
getting sick more easily
slower recovery
flare-ups of existing conditions
This is not abstract.
Emotional stress changes hormonal signaling, which in turn influences immune behavior.
Signals move continuously across systems
These interactions are not occasional.
They are constant.
Every moment:
the nervous system is signaling
hormones are adjusting
immune cells are responding
cells are adapting
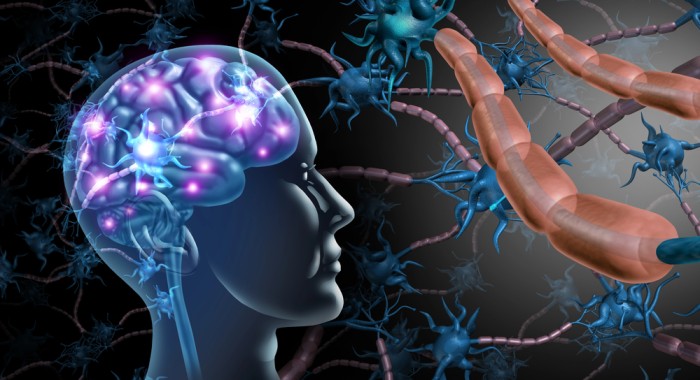
There is no true separation between systems.
There is only communication.
What This Means
The body is not a collection of independent parts.
It is a continuously communicating network, where changes in one area ripple through the entire system.
The Body Responds to Internal State
Most of us don’t need a scientific paper to recognize this.
We’ve felt it.
There are moments in life when something shifts, and the body responds immediately.
A hug from someone we love.
Laughter with a close friend.
Music that moves us.
A sense of being seen, accepted, understood.
In those moments:
breathing deepens
muscles soften
the mind quiets
This is not imagination.
It is physiology.
The nervous system shifts.
Stress signaling decreases.
The body moves toward a state of regulation.
Now consider the opposite.
Lingering resentment.
Unresolved conflict.
The replay of something that hurt us.
The body does not treat these as abstract thoughts.
It responds as if something is still wrong.
muscles tighten
sleep is disrupted
stress hormones remain elevated
Over time, these patterns are not just experiences.
They become biology.
Coherence: When the System Is in Tune
We can begin to describe health in a different way.
Not simply as the absence of disease, but as the quality of coordination within the system.
You might think of it this way:
Health is what it looks like when the body is functioning as an integrated whole — when its systems are communicating effectively, adapting appropriately, and maintaining balance under changing conditions.

Or more simply:
when every cell is, in a sense, “singing the same song” — in tune.
This is what we might call biological coherence.
It is not a single process.
It is the result of many processes working together.
How the System Evolved — and What That Means
The question naturally arises:
If this is real, and increasingly measurable, why has it not been central to how we think about health?
Part of this limitation can be traced to how modern medical education developed.
In the early 20th century, following the influence of the Flexner Report, medical education became more standardized and more grounded in laboratory science.
This brought enormous advances.
But it also shaped what the system learned to prioritize.
What the System Learned to Focus On
The system evolved around what could be clearly seen, measured, and acted upon:
Structure — What does the body look like? (bones, organs, tissues; imaging like X-rays, MRIs, CT scans)
Chemistry — What can we measure? (blood sugar, cholesterol, hormones, electrolytes)
Pathology — What is going wrong? (infection, inflammation, tissue damage, disease classification)
Intervention — What can we do about it? (medications, surgery, procedures)
This approach is powerful because it is precise, measurable, and actionable. It allows medicine to diagnose and intervene in very concrete ways.
What Received Less Emphasis
At the same time, other dimensions of human physiology — no less real, but more complex — received less emphasis in everyday clinical thinking.
These include aspects of the body that are:
Dynamic — constantly changing moment to moment (nervous system activity, stress responses, energy fluctuations)
System-wide — not confined to a single organ or pathway (brain–immune interactions, hormonal coordination, whole-body regulation)
Harder to measure — not easily captured in a single test (resilience, adaptability, the ability to return to balance)
Why This Matters
This does not mean these dimensions are unimportant.
It means they are more difficult to study within a model built around fixed measurements, isolated variables, and controlled interventions.
But living systems are not static.
They are continuously adjusting, responding, and communicating.
Which brings us back to something simple — and profound:
There is no true separation between systems.
There is only communication.
And because of that:
The body is best understood not as a collection of parts…
but as a continuously communicating network, where changes in one area ripple through the entire system.
Chronic Disease Is Different
Many physicians are just as frustrated as their patients with the limits of managing chronic disease. They see:
- conditions that persist despite treatment
- symptoms that are controlled but not resolved
- patients who never fully regain their health
The current approach to chronic disease is not delivering the outcomes that patients or physicians are looking for.
Part of this limitation can be traced to how modern medical education developed.
Shaped in large part by the legacy of the Flexner Report, it was built around acute care, trauma, infection, and conditions that require immediate intervention.
For these problems, the model works extremely well.
Chronic disease is different.
It is not typically the result of a single event or isolated malfunction.
It reflects a gradual breakdown in system-wide regulation — across metabolism, immune function, hormones, and nervous system signaling.

And the tools designed for acute intervention do not fully translate to restoring that level of function.
Chronic disease is not primarily a problem of missing interventions.
It is a problem of missing models.
This is not a failure of the physician.
It is a limitation of the system, and the model on which it is based.
A Necessary Evolution
What is needed is not more effort within the same framework, but an expansion of that framework.
A shift toward:
systems biology
functional understanding
restoration of regulatory balance
Doctors and practitioners in natural and functional medicine have long worked in this way, focusing on how systems interact and how function can be restored rather than simply managed.
The next step is clear:
to incorporate this systems biology training into mainstream medical education and practice, so that physicians are equipped with tools that match the reality of chronic disease.
A Shared Responsibility
This is not a change that belongs to physicians alone.
It belongs to all of us.
Patients and doctors together have a role to play in asking better questions, seeking better tools, and supporting the evolution of a system that reflects how the human body actually works.
Because when the model matches the problem, outcomes improve.
The Invitation
This series is about expanding the lens through which we understand health.
Because once we begin to see the body as a coordinated, adaptive system — one influenced not only by external inputs but by internal states — we begin to see something else as well:
We are not passive participants in our health.
We are participants in an ongoing process of regulation, adaptation, and response.
The body is not only shaped by what happens to it.
It is shaped by how it experiences and responds to those events.
And that changes the conversation.
— End of Part 1 —